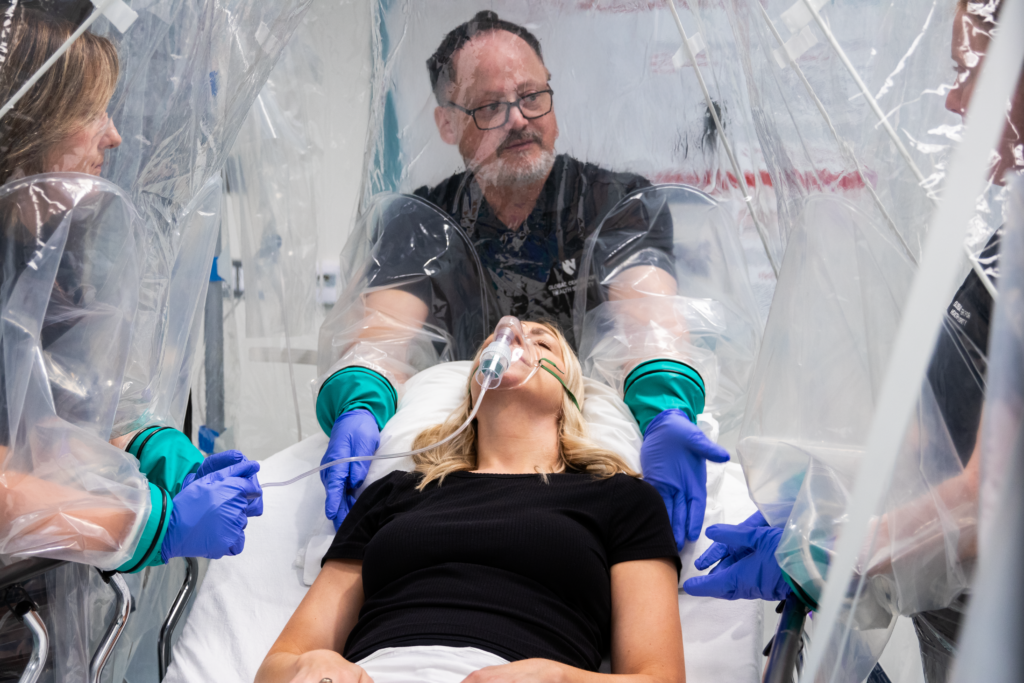
Carecubes demonstrates a viable model for medtech innovation addressing critical infrastructure gaps exacerbated by recent global health crises. The startup’s FDA-cleared isolation system, transforming standard hospital beds into deployable units within minutes, directly tackles the escalating costs and limitations of traditional personal protective equipment (PPE) strategies. This scalable solution has achieved significant commercial traction, with installations in over 36 U.S. communities across 13 states and territories, validating both the technology’s utility and market demand in high-stress healthcare environments. The successful $6.5 million Series A financing round, led by specialized healthcare investors including Schooner Capital and Lifeforce Capital, underscores institutional confidence in the company’s potential to mitigate infectious disease containment challenges, providing a blueprint for sustainable venture capital deployment in critical infrastructure innovation.
The funding structure for Carecubes highlights the importance of strategic capital allocation in medtech development. The diverse investor base, encompassing dedicated healthcare venture firms and industry-affiliated partners, reflects a multi-faceted approach to de-risking and scaling health technology. This model, emphasizing both financial capital and operational mentorship, offers valuable insights for regional development. By leveraging grants initially and transitioning to targeted venture investment, Carecubes exemplifies how tailored capital strategies can bridge the gap between research and commercialization, particularly crucial in sectors facing persistent underinvestment like regional healthcare infrastructure.
Beyond its immediate commercial success, Carecubes’ evolution from pandemic-era necessity to a product addressing chronic healthcare system strain reveals profound implications for regional infrastructure resilience. The modular isolation units’ ability to reduce supply chain dependency on single-use PPE, optimize hospital bed utilization, and enhance caregiver safety directly mitigates operational inefficiencies and costs. This principle translates readily to the MENA region, where similar pressures on primary healthcare systems, surge capacity limitations, and the need for adaptable containment solutions during outbreaks are acute. Investments in scalable, locally manufacturable isolation and containment technologies, supported by strategic regional venture capital and sovereign risk-sharing mechanisms, represent a critical infrastructure investment with potential to enhance public health security and reduce long-term systemic costs across diverse healthcare delivery models.